What Is Hyperbaric Oxygen Therapy Used For? The 14 FDA Indications Explained
Most people encounter the therapy for the first time after a carbon monoxide emergency or a diving accident. But the therapy is used for 14 formally recognised conditions — and CO poisoning is only one of them.

what is hyperbaric oxygen therapy used for — 14 FDA indications carbon monoxide poisoning HBOT
What is hyperbaric oxygen therapy used for? The short answer is 14 conditions — each recognised by the US Food and Drug Administration and the Undersea and Hyperbaric Medical Society.
The longer answer starts with carbon monoxide poisoning. CO poisoning is the condition that best illustrates why the therapy exists — and what it does that no other treatment can replicate. Understanding CO poisoning as the emergency benchmark makes every other indication easier to understand.
This article covers the full list — all 14 FDA-recognised uses of the therapy — with the mechanism, the evidence, and the India-specific context for each. It is the complete guide for patients, families, and clinicians asking the foundational question.
For the detailed CO poisoning treatment evidence, see our article on carbon monoxide poisoning and HBOT brain protection. For the foundational mechanism, visit How HBOT Works.
Hyperbaric oxygen therapy (HBOT): A treatment in which a patient breathes 100% pure oxygen inside a pressurised chamber at 1.5 to 3.0 times normal atmospheric pressure. The increased pressure causes oxygen to dissolve directly into blood plasma — reaching tissue through diffusion independent of haemoglobin and normal circulation. Used for 14 FDA-recognised indications across emergency, wound care, neurological, and infection categories.
What Is Hyperbaric Oxygen Therapy Used For — Starting With CO Poisoning
Carbon monoxide poisoning is the condition that makes the mechanism of HBOT most vivid. CO binds to haemoglobin 250 times more tightly than oxygen — displacing it from the molecule that carries oxygen to every cell in the body. The result is cellular suffocation. The heart is beating. The lungs are working. But oxygen cannot reach the tissue that needs it.
Standard treatment — breathing high-flow oxygen at normal pressure — displaces CO from haemoglobin at a rate that takes several hours. HBOT at 2.5 ATA displaces it dramatically faster, in a fraction of the time. More importantly, HBOT also displaces CO from cytochrome c oxidase — the mitochondrial enzyme responsible for cellular energy production — preventing the delayed neurological syndrome that standard oxygen therapy does not address.
The delayed neurological syndrome after CO poisoning — which can manifest weeks later as cognitive decline, personality change, and motor dysfunction — is prevented by HBOT in approximately 50% of cases where it develops without treatment. confirmed the mitochondrial protection mechanism that makes HBOT uniquely effective for CO exposure.
CO poisoning is HBOT’s emergency benchmark because it illustrates the core mechanism most clearly: oxygen delivered under pressure reaches tissue through pathways that normal haemoglobin transport cannot — and changes outcomes that standard treatment leaves unaddressed.
What Is Hyperbaric Oxygen Therapy Used For — All 14 FDA Indications
The 14 FDA and UHMS-recognised indications for HBOT fall into four broad categories: emergency conditions, wound healing, infection, and radiation injury. Each shares the same fundamental mechanism — delivering therapeutic oxygen to tissue that cannot receive adequate oxygen through normal circulation.
| # | Indication | Primary Mechanism | Full Article |
| 01 | Diabetic foot wounds and non-healing ulcers | Plasma oxygenation + angiogenesis restores healing in hypoxic tissue | hbotlab.com/hbot-diabetic-foot-wound-healing/ |
| 02 | Decompression sickness (the bends) | Boyle’s Law compresses nitrogen bubbles; plasma O₂ restores tissue | hbotlab.com/decompression-sickness-hbot-treatment/ |
| 03 | Carbon monoxide poisoning | Displaces CO from haemoglobin and mitochondria; prevents DNS | hbotlab.com/carbon-monoxide-poisoning-hbot-brain-protection/ |
| 04 | Gas gangrene (clostridial myonecrosis) | Direct bactericidal against anaerobes; toxin suppression | hbotlab.com/hbot-gas-gangrene-clostridial-myonecrosis/ |
| 05 | Radiation injury — late tissue effects | Angiogenesis in hypovascular radiated tissue; fibroblast reactivation | hbotlab.com/hbot-radiation-injury-cancer-survivors/ |
| 06 | Crush injuries and compartment syndrome | Plasma O₂ without blood flow; reperfusion injury modulation | hbotlab.com/hbot-crush-injury-compartment-syndrome/ |
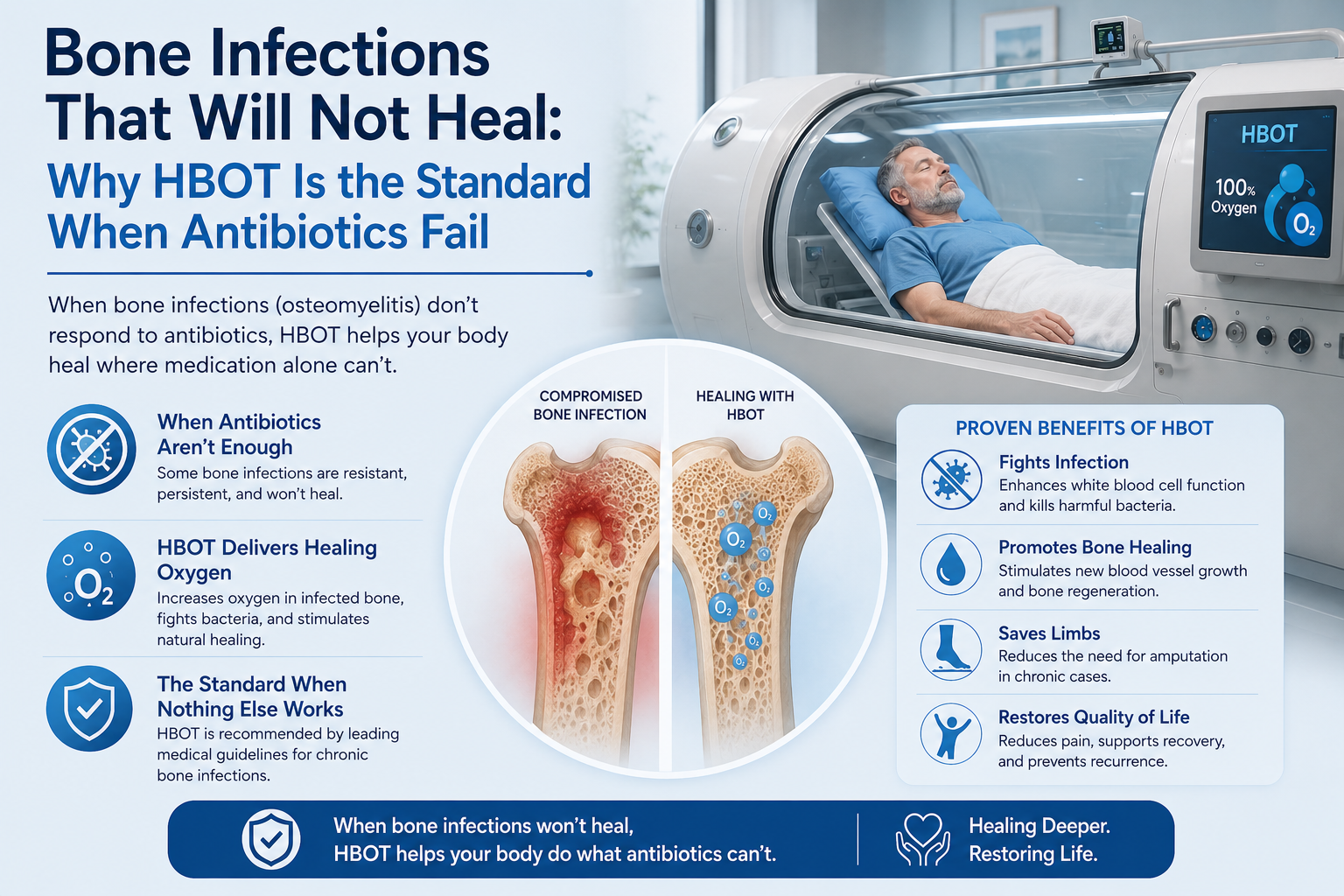
| 07 | Refractory osteomyelitis | Antibiotic potentiation; leukocyte restoration; biofilm disruption | hbotlab.com/hbot-refractory-osteomyelitis-bone-infection/ |
| 08 | Necrotising soft tissue infections | Direct anaerobic bactericidal; toxin suppression; leukocyte potentiation | hbotlab.com/hbot-necrotising-fasciitis-survival/ |
| 09 | Acute arterial insufficiency | Plasma diffusion oxygenation without functional circulation | hbotlab.com/hbot-acute-arterial-insufficiency/ |
| 10 | Arterial gas embolism | Boyle’s Law bubble compression; gas reabsorption acceleration | hbotlab.com/arterial-gas-embolism-hbot-treatment/ |
| 11 | Severe anaemia — no transfusion | Plasma O₂ replaces haemoglobin transport; bridge to recovery | hbotlab.com/hbot-severe-anaemia-no-transfusion/ |
| 12 | Thermal burns | Zone of stasis preservation; anti-inflammatory; angiogenesis | hbotlab.com/hbot-burns-healing-recovery/ |
| 13 | Intracranial abscess | Antibiotic potentiation; neurological tissue oxygenation | hbotlab.com/hbot-brain-abscess-recovery/ |
| 14 | Compromised skin grafts and flaps | Graft bed oxygenation; angiogenesis; anti-infective | hbotlab.com/hbot-skin-therapy-grafts-flaps/ |
| One mechanism — 14 applications | Every FDA-recognised use of hyperbaric oxygen therapy works through the same biological foundation: increased plasma-dissolved oxygen under pressure reaching tissue through diffusion. The 14 indications differ in which tissue is hypoxic and what biological process the restored oxygen enables — but the underlying mechanism is identical across all of them. |
Why CO Poisoning Illuminates What HBOT Is Used For Across All Indications
CO poisoning earns its place as the emergency benchmark not just because it is life-threatening — but because it demonstrates the three mechanisms that all 14 indications depend on.
Mechanism 1 — Plasma Oxygenation Independent of Haemoglobin
In CO poisoning, haemoglobin is occupied — bound to CO and unable to carry oxygen. HBOT oxygenates tissue through plasma dissolution, completely bypassing the blocked haemoglobin. This same plasma oxygenation mechanism is what makes HBOT useful in arterial insufficiency, severe anaemia, crush injury, and every other condition where normal oxygen delivery is compromised.
Mechanism 2 — Reaching Tissue Through Diffusion
The plasma-dissolved oxygen created by HBOT travels through tissue by diffusion — not through blood vessels. This means it reaches hypoxic tissue even when the vessels supplying that tissue are blocked, damaged, or destroyed. This is the mechanism behind HBOT’s effectiveness in diabetic wounds, radiation injury, osteomyelitis, and graft failure — all conditions where the problem is not a lack of oxygen in the blood, but a failure to deliver it to the tissue that needs it.
Mechanism 3 — Biological Cascade Activation
Beyond immediate oxygenation, HBOT triggers the biological cascades that repair damaged tissue — angiogenesis, stem cell mobilisation, inflammatory modulation. documented the 8-fold increase in circulating stem cells with HBOT — a repair mechanism triggered by the therapy that extends its benefit beyond the session itself. This cascade activation is what makes HBOT a lasting treatment rather than a temporary support.
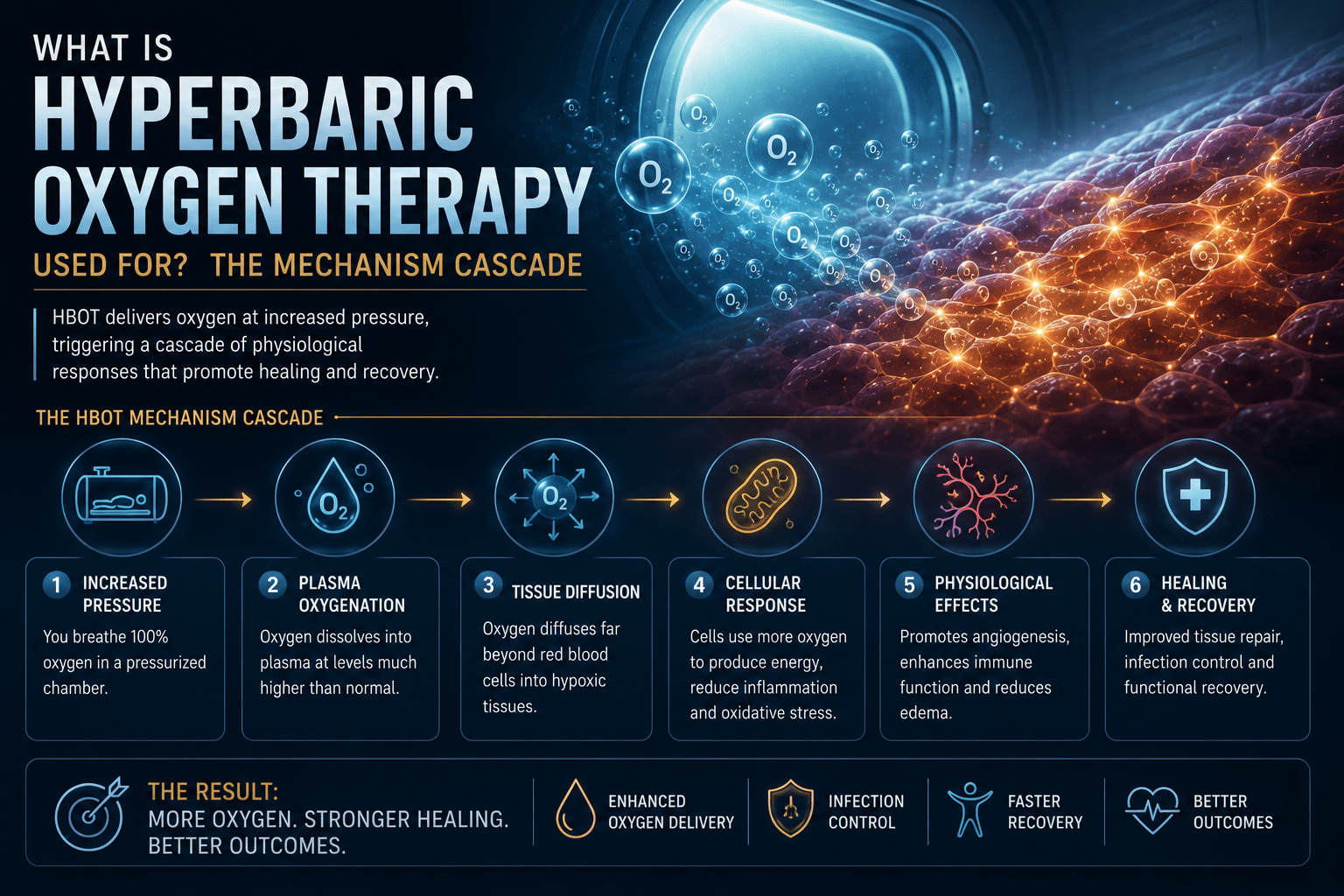
what is hyperbaric oxygen therapy used for — mechanism plasma oxygenation diffusion cascade
What Is HBOT Used For in India — The Most Relevant Indications
Of the 14 FDA-recognised uses of hyperbaric oxygen therapy, four carry particular clinical urgency in the Indian context.
Carbon Monoxide Poisoning — India’s Silent Epidemic
CO poisoning from gas heaters, coal fires, and generator exhaust is a significant cause of preventable death in India — particularly during winter months in North India. Awareness that HBOT is the definitive treatment, rather than standard oxygen therapy alone, remains extremely low among Indian emergency physicians and families.
Diabetic Wounds — India’s Largest HBOT Patient Population
With 77 million diabetics, India has the world’s second-largest diabetic population. Non-healing foot ulcers and amputation prevention represent the single largest volume of HBOT-eligible patients in the country. HBOT for diabetic wounds is the most clinically impactful use of the therapy in the Indian context.
For the complete diabetic wound evidence, see our guide on HBOT for diabetic foot wounds and our safety guide on HBOT benefits and risks for diabetic patients.
Necrotising Fasciitis — India’s High-Incidence Emergency
India’s tropical climate, high rates of diabetes, and varying wound hygiene access create a high-incidence environment for necrotising soft tissue infections. HBOT reduces mortality by nearly half in documented evidence — yet awareness among Indian emergency surgeons remains limited.
Decompression Sickness — India’s Growing Dive Community
The Andaman Islands, Lakshadweep, and coastal India’s growing dive industry create an increasing DCS burden. Most Indian dive sites are hours from the nearest hyperbaric facility.
For HBOT facility locations across India, see our guides to HBOT in Delhi and HBOT in Bangalore. For a national guide, visit our HBOT near me India guide.
Frequently Asked Questions
Is HBOT only used for emergencies?
No. Of the 14 FDA-recognised uses, approximately half are emergency or acute conditions (CO poisoning, DCS, gas gangrene, arterial gas embolism, necrotising fasciitis, crush injury, arterial insufficiency) and half are chronic or subacute conditions (diabetic wounds, radiation injury, osteomyelitis, burns, brain abscess, skin grafts, severe anaemia). HBOT is used across the full spectrum from emergency to elective wound management.
What conditions is HBOT NOT used for?
The therapy does not have FDA recognition for stroke, autism, cancer (as primary treatment), anti-ageing, or general wellness — though research into some of these applications is ongoing and some are used off-label in certain clinical contexts. The 14 FDA-recognised indications are where the evidence is strongest and the clinical rationale is most established. HBOTLAB covers the evidence for emerging applications honestly in the Knowledge Centre.
How do I know if my condition qualifies for HBOT?
The 14 FDA-recognised indications in the table above are the starting point. If your condition appears in the list, you are eligible for a formal clinical assessment. HBOT should be prescribed by a qualified hyperbaric physician — not self-administered or initiated without medical oversight. A referral from your treating specialist to a hyperbaric facility is the appropriate pathway.
What is hyperbaric oxygen therapy used for most often in Indian hospitals?
The three most common indications in Indian hospital-based hyperbaric units are diabetic foot ulcers, non-healing wounds in post-radiation patients, and refractory osteomyelitis. Emergency indications — CO poisoning, DCS, gas gangrene — are treated acutely but represent smaller volume than the chronic wound indications.
Where can I read about each indication in detail?
The HBOTLAB Knowledge Centre has a dedicated article for every one of the 14 FDA-recognised indications. The full conditions reference is at our HBOT conditions section.
Fourteen Uses. One Mechanism. One Question That Matters.
What is hyperbaric oxygen therapy used for? It is used for 14 conditions where tissue is hypoxic — where the oxygen that the body needs to fight infection, heal wounds, repair nerves, or recover from poisoning cannot be delivered through normal circulation.
Carbon monoxide poisoning illustrates the mechanism most vividly because the haemoglobin failure is sudden and complete. But every other indication on the list has the same underlying problem — tissue that is not receiving the oxygen it needs to function, heal, or survive. HBOT addresses that problem directly, through physics rather than pharmacology.
For Indian patients and families — the question of whether your condition is one that HBOT is used for starts with this list. If it appears above, the evidence exists, the protocol is established, and access in India is available.
For the complete mechanism explanation, visit How HBOT Works. For the full conditions evidence base, explore the HBOT conditions section.





[…] For the foundational mechanism of how HBOT oxygenates hypoxic tissue, visit How HBOT Works. For the full 14-indication overview, see our HBOT uses guide. […]