HBOT Treatment for Gas Gangrene: The Three Mechanisms That Change Survival Outcomes
Gas gangrene creates three simultaneous biological crises. Bacteria spread. Toxins destroy. Immune function fails. Surgery addresses one. HBOT treatment addresses all three — in the same session.

hbot treatment gas gangrene — three mechanisms survival clostridial myonecrosis hyperbaric oxygen
HBOT treatment for gas gangrene does something that surgery and antibiotics cannot do alone.
Gas gangrene — clostridial myonecrosis — is one of the fastest-moving tissue infections in medicine. The bacteria spread at several centimetres per hour. The toxins they produce destroy muscle independently of bacterial count. And the environment they create — profoundly anaerobic, hypoxic tissue — actively supports their growth and impairs every immune defence the body has.
Surgery removes infected tissue. Antibiotics reduce bacterial load. Both are essential and non-negotiable. But neither restores oxygen to the tissue that allows Clostridia to thrive and toxins to go unsuppressed.
HBOT treatment addresses that oxygen environment directly. The result is documented reduction in mortality and amputation rate — making it one of the most evidence-supported adjunctive therapies in emergency infectious disease medicine.
For the full clinical evidence on gas gangrene and HBOT outcomes, see our primary guide on HBOT for gas gangrene and clostridial myonecrosis. For the foundational oxygen delivery mechanism, visit How HBOT Works.
Gas gangrene (clostridial myonecrosis): A rapidly progressive soft tissue infection caused by Clostridium species — anaerobic bacteria that thrive in oxygen-deprived tissue. Produces alpha-toxin and other myotoxins that destroy muscle at speed. Mortality without surgical treatment: 100%. With surgery alone: 20-30%. With surgery plus HBOT treatment: documented reduction to single figures in centres with rapid access to all three modalities.
Why Gas Gangrene Resists Standard Treatment Alone
Understanding why surgery and antibiotics alone produce 20-30% mortality — despite aggressive intervention — requires understanding the three simultaneous biological crises gas gangrene creates.
Crisis 1 — The Anaerobic Environment
Clostridia are obligate anaerobes — they die in the presence of oxygen. But the tissue they infect becomes progressively more hypoxic as they damage the microvascular supply. The infection creates the exact environment it needs to survive: destroying the oxygen delivery that would kill it.
Surgery removes infected tissue — but cannot reoxygenate the viable tissue at the wound margins that is becoming progressively more anaerobic. Without oxygen restoration, marginal tissue continues to support bacterial growth even after debridement.
Crisis 2 — Alpha-Toxin Production
Alpha-toxin — the primary virulence factor of Clostridium perfringens — is produced continuously and destroys cell membranes, causing haemolysis and direct tissue necrosis. Alpha-toxin production is suppressed in aerobic environments. In anaerobic tissue it is produced at maximum rate.
Antibiotics reduce bacterial load. They do not block toxin production from living organisms. In anaerobic tissue, toxins are produced faster than they can be cleared.
Crisis 3 — Impaired Leukocyte Function
Leukocyte killing requires tissue oxygen tension above 30 mmHg. The tissue oxygen tension in gas gangrene is close to zero. Immune cells that arrive at the infection site cannot mount their full killing response because the environment has disabled it.
| Biological Crisis | What Happens Without HBOT | What HBOT Treatment Does |
| Anaerobic environment | Bacteria thrive at wound margins after surgery; re-infection risk persists | Raises tissue O₂ to bactericidal levels — directly toxic to Clostridia |
| Alpha-toxin production | Toxins continue destroying tissue independently of antibiotic effect | High O₂ environment suppresses toxin synthesis; documented 50% alpha-toxin reduction |
| Impaired leukocyte function | Immune cells present but cannot kill in hypoxic tissue | Restores tissue O₂ above 30 mmHg — full leukocyte bactericidal function restored |
HBOT treatment does not replace surgery or antibiotics. It addresses the layer beneath them — the oxygen environment that determines whether bacteria survive after debridement, whether toxins continue, and whether the immune system can function.
HBOT Treatment Mechanism 1 — Direct Bactericidal Action Against Clostridia
Clostridium perfringens and other gas gangrene pathogens are obligate anaerobes. At tissue oxygen tensions achieved by HBOT treatment — above 200 mmHg during sessions — they cannot survive.
confirmed that HBOT creates tissue oxygen concentrations directly lethal to obligate anaerobes — producing an environment in which continued bacterial growth at the wound margin is no longer possible. This effect persists between sessions as tissue oxygen levels remain elevated above pre-treatment baseline.
The clinical significance: surgery removes the bulk of infected tissue. HBOT treatment sterilises the margins — the viable tissue adjacent to the debridement zone that carries the residual bacterial load responsible for recurrence.
HBOT Treatment Mechanism 2 — Alpha-Toxin Suppression
documented that HBOT significantly reduces Clostridial toxin production — with measured reductions of approximately 50% in alpha-toxin levels in tissue exposed to therapeutic oxygen pressures.
This toxin suppression mechanism is distinct from the bactericidal effect. Even before bacteria are killed, the tissue-destructive toxins they produce are being suppressed — reducing ongoing necrosis that continues independently of bacterial count.
The practical implication: the window between HBOT sessions is not a treatment gap. Tissue oxygen remains elevated for several hours after each session — continuing to suppress toxin production even when the patient is not in the chamber.
HBOT Treatment Mechanism 3 — Leukocyte Potentiation
The third mechanism restores the immune function the anaerobic environment has disabled. HBOT raises tissue oxygen tension above the 30 mmHg threshold that leukocyte killing requires — restoring the immune system’s bactericidal function in the infected tissue.
documented that the combination of restored leukocyte function and antibiotic therapy produces substantially better bactericidal outcomes than either alone — confirming that HBOT treatment and antibiotics work through different, complementary mechanisms.
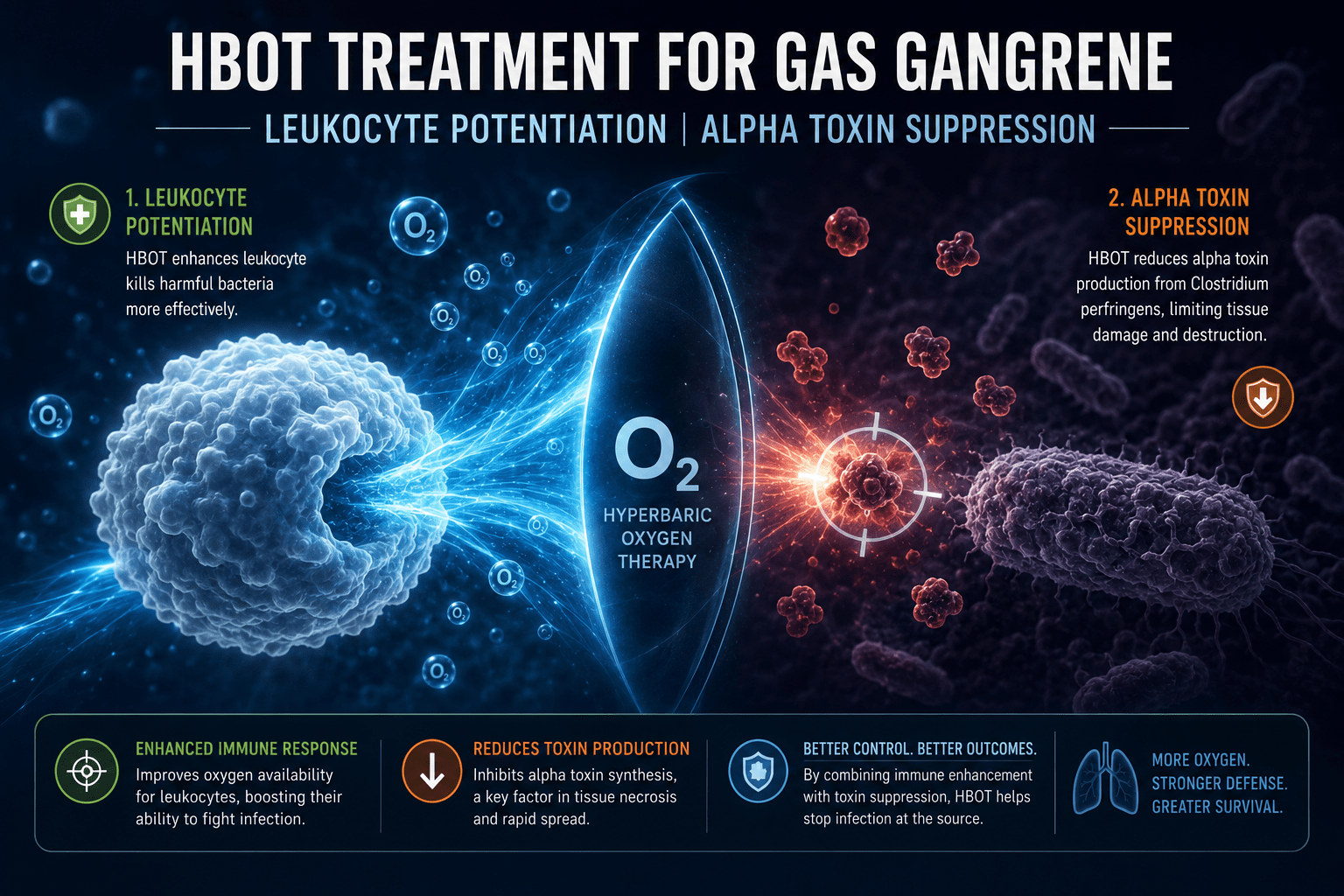
hbot treatment gas gangrene — leukocyte potentiation alpha toxin suppression mechanism
The Evidence Behind HBOT Treatment for Gas Gangrene
| Mortality Data | Surgery alone for gas gangrene: 20-30% mortality. Surgery plus antibiotics plus HBOT treatment: 5-10% mortality in centres with rapid access to all three modalities. The difference is most pronounced in truncal involvement — where radical debridement is anatomically limited and HBOT’s ability to sterilise margins without further tissue loss is most valuable. |
confirmed gas gangrene as a well-established HBOT indication with documented survival benefit when added to standard surgical and antibiotic management. The evidence base spans more than five decades of clinical series.
HBOT Treatment Protocol for Gas Gangrene
Standard Parameters
- Pressure: 2.5 to 3.0 ATA — higher than most indications to maximise anaerobic bactericidal effect
- Session duration: 90 minutes at target pressure
- Frequency: 3 sessions in first 24 hours — then twice daily until infection is controlled
- Concurrent treatment: surgical debridement and antibiotics are mandatory — HBOT is adjunctive
- Timing: first session should follow immediately after initial surgical debridement
Why Three Sessions in 24 Hours
The first 24 hours are the period of maximum bacterial proliferation and toxin production. Three HBOT sessions in this window — separated by approximately 6 to 8 hours — maintain elevated tissue oxygen levels through the full first day, suppressing toxins and sterilising margins during the period when re-infection risk from residual bacteria is highest.
HBOT Treatment for Gas Gangrene in India
Gas gangrene in India presents most commonly following agricultural injuries, road traffic accidents, and post-surgical infections. The combination of soil contamination, delayed presentation, and limited awareness of HBOT as adjunctive treatment produces mortality outcomes significantly above what is achievable with optimised combined management.
The single most important factor in gas gangrene outcomes is time. Every hour from diagnosis to HBOT initiation allows bacterial spread and toxin accumulation that no subsequent treatment can reverse.
For the related evidence on HBOT in necrotising fasciitis — which shares the anaerobic mechanism — see our guide on HBOT for necrotising fasciitis. For the infection osteomyelitis indication, see our article on HBOT for refractory osteomyelitis.
For HBOT facility locations in India, see our guides to HBOT in Delhi and HBOT in Bangalore. For a national guide, visit our HBOT near me India guide.
Frequently Asked Questions
Can HBOT treatment replace surgery for gas gangrene?
No. Surgical debridement is non-negotiable — it removes the bacterial mass and necrotic tissue that HBOT cannot address. The combination of surgery, antibiotics, and HBOT produces the best documented outcomes. Withholding any of the three worsens mortality.
How quickly must HBOT treatment begin after diagnosis?
Within 6 hours of diagnosis for maximum benefit. The bacterial spread rate means every hour of delay allows progressive tissue destruction. The first HBOT session should follow immediately after the initial surgical procedure.
How many HBOT sessions are needed?
Typically 10 to 15 sessions over 5 to 7 days. Three sessions in the first 24 hours, then twice daily until infection is clinically controlled — no further tissue spread, reducing inflammatory markers, improving wound appearance.
Is HBOT treatment covered by insurance for gas gangrene in India?
Coverage varies by insurer and policy. For current guidance see our dedicated article on HBOT insurance coverage in India.
What is the difference between gas gangrene and necrotising fasciitis?
Gas gangrene is caused specifically by Clostridium species and affects primarily muscle. Necrotising fasciitis affects the fascia and soft tissue and is usually caused by mixed organisms. Both benefit from HBOT treatment through the same mechanisms — anaerobic bactericidal action, toxin suppression, and leukocyte potentiation. Gas gangrene typically spreads faster and carries higher acute mortality.
Three Crises. One Treatment That Addresses All Three.
Gas gangrene creates three simultaneous biological crises: bacteria that thrive in the environment they create, toxins that destroy tissue independently of bacterial count, and an immune system disabled by hypoxia.
Surgery addresses one — removing infected tissue. Antibiotics address one — reducing bacterial load. HBOT treatment addresses all three — sterilising margins, suppressing toxin production, and restoring immune function.
The mortality difference between surgery alone and surgery plus HBOT treatment is not marginal. It is the difference between 20-30% and single figures. For a condition that kills in hours, that difference is measured in lives.
The survival data for gas gangrene with combined treatment is among the strongest in emergency infectious disease medicine. The three-mechanism model explains why: each treatment addresses a different layer of the infection. No single modality addresses all three. The combination is what produces the outcome.
For the full gas gangrene treatment evidence, see our primary guide on HBOT for gas gangrene and clostridial myonecrosis. For all 14 FDA indications, see our HBOT treatment uses guide.
Three crises. Three mechanisms. One HBOT treatment session addressing all simultaneously.