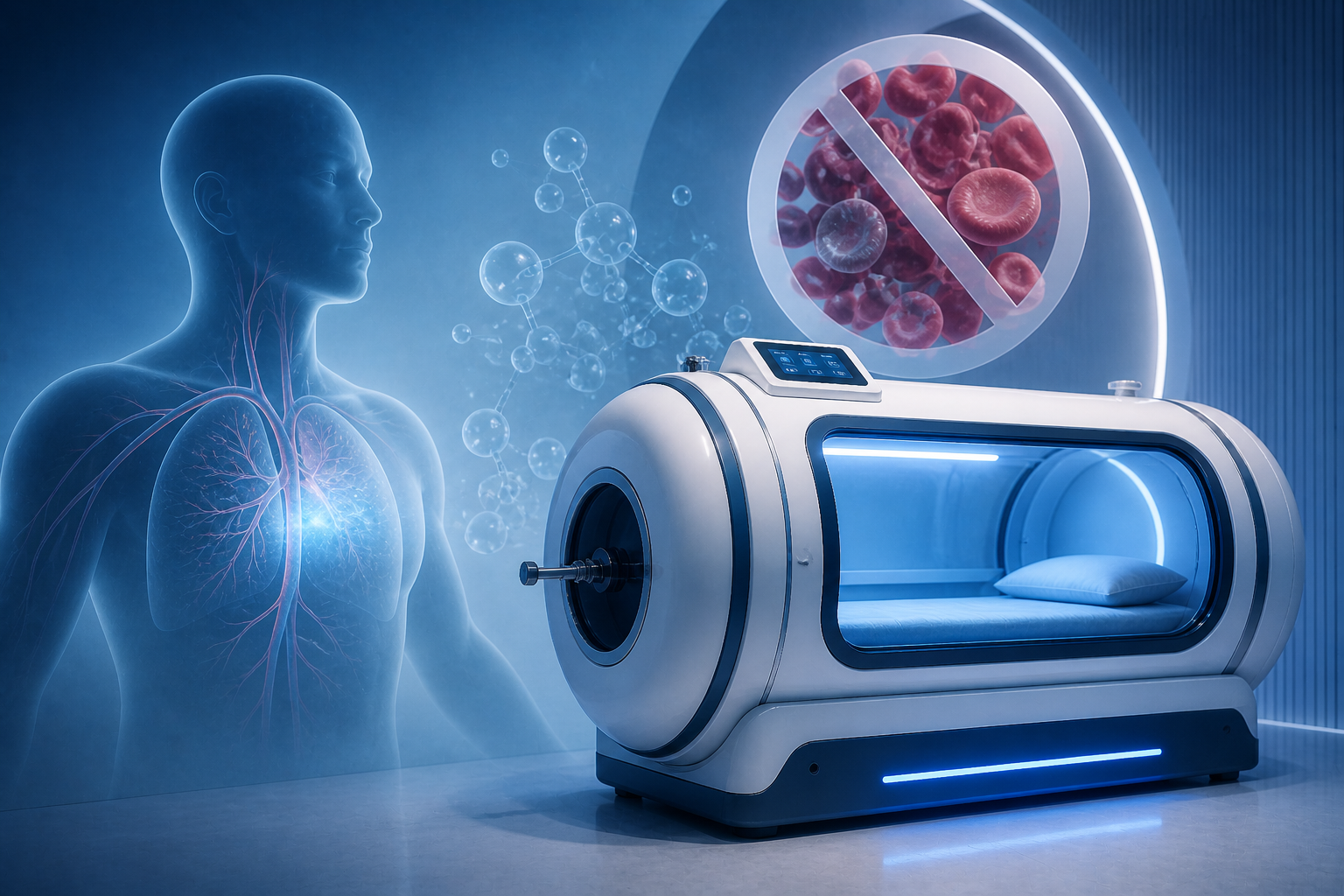
When Blood Transfusion Is Refused or Impossible: How HBOT Keeps Tissue Alive
At 2.0 to 2.4 ATA, blood plasma carries enough dissolved oxygen to meet resting tissue requirements without haemoglobin. When transfusion is impossible, this is not a theoretical option — it is a documented, UHMS-recognised bridge to survival.
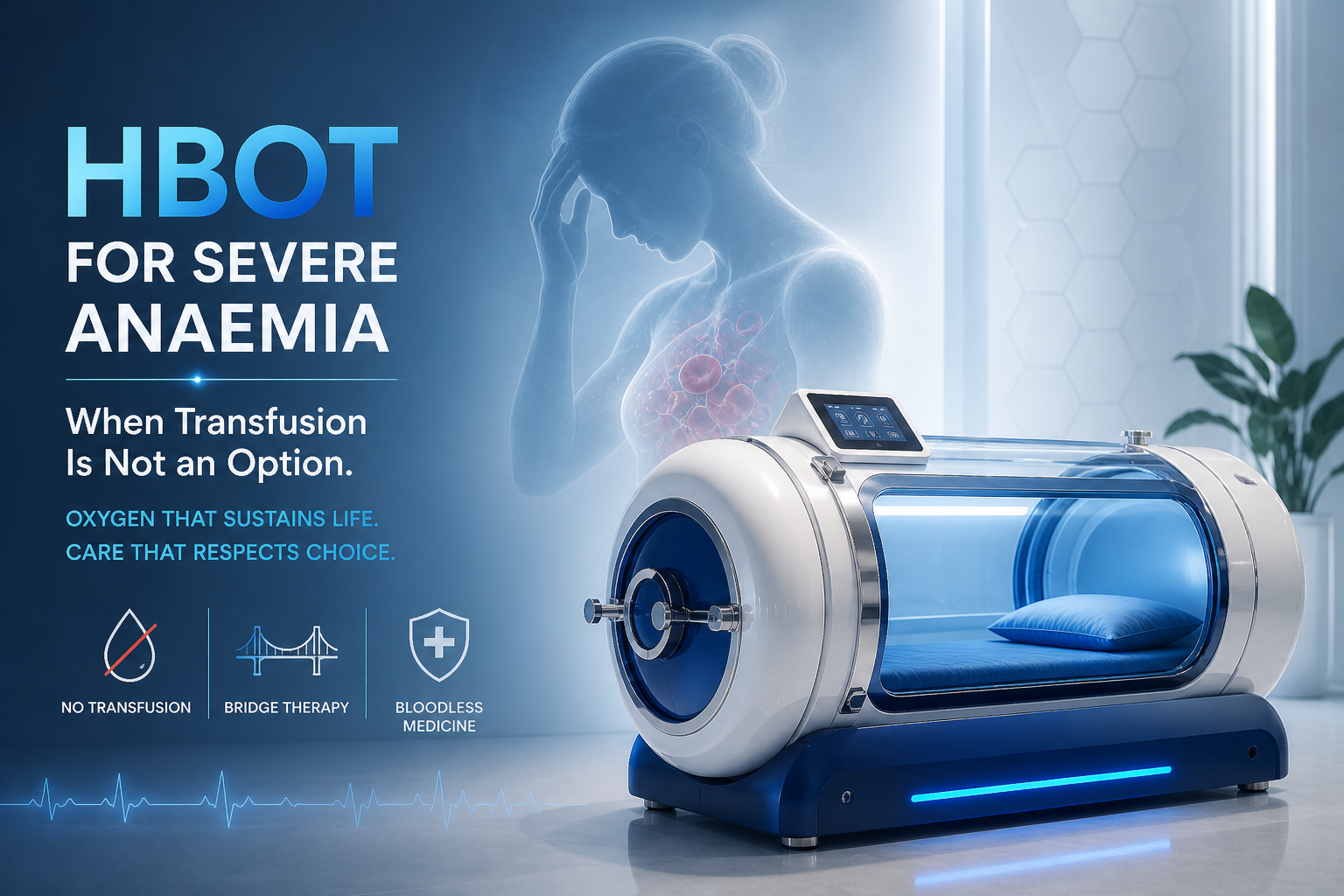
HBOT severe anaemia no transfusion — hyperbaric oxygen therapy bridge bloodless medicine
This article addresses two distinct situations where transfusion is not possible: medical contraindication, and personal or religious refusal. Both are treated with equal clinical respect throughout. HBOT is presented as a medically sound option — not a compromise, not an alternative to faith, and not a last resort. It is a recognised therapy that medicine itself has developed for precisely this situation.
The blood loss is severe. The haemoglobin is critically low. And for this patient, in this moment, a blood transfusion is not possible.
It may be a medical reason — a rare antibody making compatible blood unavailable, a haemolytic reaction risk, a clinical contraindication. Or it may be a deeply held personal belief — a conviction that has been part of this person’s life and identity long before they ever imagined needing surgery.
Whatever the reason, the clinical challenge is the same. Tissue is not receiving the oxygen it needs. The body cannot wait indefinitely for haemoglobin to recover through natural erythropoiesis. Something must bridge the gap between now and recovery.
HBOT is that bridge. Not as a compromise. Not as a desperate measure. As a formally recognised therapy — acknowledged by the Undersea and Hyperbaric Medical Society, supported by the physics of Henry’s Law, and used in bloodless medicine programmes at major hospital centres globally.
The mechanism that makes HBOT work here is the same one that makes it effective across all its vascular indications — plasma-dissolved oxygenation. The physics is explained fully at How HBOT Works.
The Oxygen Delivery Crisis in Severe Anaemia
Understanding why severe anaemia is life-threatening requires understanding how oxygen is normally transported in blood — and what happens when that transport system fails.
Normal Oxygen Transport — The Haemoglobin Dependency
Under normal conditions, approximately 98% of oxygen in the blood is carried by haemoglobin — the iron-containing protein in red blood cells. Each haemoglobin molecule carries four oxygen molecules, released to tissue as blood passes through capillary beds.
The remaining 2% — approximately 0.3 ml O₂ per 100 ml blood — is dissolved in plasma. This contribution is functionally negligible under normal circumstances. Tissue at rest requires approximately 5 to 6 ml O₂ per 100 ml blood. Haemoglobin provides virtually all of it.
When haemoglobin falls to critically low levels — through acute blood loss, haemolysis, or bone marrow failure — the oxygen transport system collapses. Tissue begins to receive insufficient oxygen. Cellular energy production fails. Organs begin to shut down in order of their oxygen sensitivity.
The Physiological Cascade of Severe Anaemia
| Haemoglobin Level | Physiological Status | Tissue Oxygen Delivery |
|---|---|---|
| 12–16 g/dL (normal) | Full oxygen transport capacity | Adequate for all metabolic demands |
| 8–10 g/dL (mild anaemia) | Compensated — heart rate and output increase | Adequate at rest; limited during exertion |
| 6–8 g/dL (moderate anaemia) | Significant compensation required | Marginally adequate at rest; tissue hypoxia on activity |
| 4–6 g/dL (severe anaemia) | Maximal cardiovascular compensation | Insufficient — critical organs begin to experience hypoxia |
| Below 4 g/dL (critical anaemia) | Compensation failing | Life-threatening — brain, heart, kidney under severe hypoxia |
| Below 2 g/dL (extreme anaemia) | Cardiovascular collapse imminent | Incompatible with survival without intervention |
How HBOT Bypasses the Haemoglobin Requirement
Henry’s Law is the physical foundation. The amount of gas dissolved in a liquid is proportional to the partial pressure of that gas above the liquid. At increased atmospheric pressure, more oxygen dissolves into blood plasma — independent of haemoglobin.
| The Numbers | At 1.0 ATA breathing air: plasma carries 0.3 ml O₂ per 100 ml blood. At 2.0 ATA breathing 100% oxygen: plasma carries 4.4 ml O₂ per 100 ml blood. At 2.4 ATA: plasma carries approximately 6.0 ml O₂ per 100 ml blood — sufficient to meet resting tissue oxygen requirements without any haemoglobin contribution. The haemoglobin is depleted. The plasma, under pressure, carries enough oxygen to sustain life. |
This is not theoretical. documented that at 3.0 ATA, plasma-dissolved oxygen is sufficient to support life in a completely haemoglobin-free preparation — a finding that has been replicated and confirmed across subsequent research.
For a patient with severe anaemia — whose haemoglobin may be 3 or 4 g/dL rather than zero — each HBOT session provides enough plasma-dissolved oxygen to sustain tissue viability at rest during the critical window when haemoglobin is recovering.
The sessions are temporary — plasma oxygen returns toward baseline between sessions. But they sustain tissue viability long enough for erythropoiesis, iron supplementation, or surgical haemostasis to begin restoring haemoglobin toward functional levels.
HBOT does not cure anaemia. It bridges the gap between critically low haemoglobin and the time required for the body or for medicine to restore it. That bridge can be the difference between survival and organ failure.
HBOT in Bloodless Medicine — Where It Fits
Bloodless medicine is a clinical discipline that has developed over decades — originally in response to the needs of Jehovah’s Witness patients, now embraced as a quality standard for all patients seeking to minimise or avoid transfusion.
Modern bloodless medicine programmes use a combination of strategies to manage severe anaemia without transfusion. HBOT is one component of this combination — not the entire protocol, but a critical bridge element that no other strategy replicates.
The Bloodless Medicine Toolkit
- Erythropoiesis-stimulating agents (EPO) — stimulate red blood cell production. Effective but require days to weeks for meaningful haemoglobin recovery.
- Intravenous iron therapy — provides the substrate for erythropoiesis. Complements EPO but does not produce immediate oxygen delivery improvement.
- Cell salvage (autologous blood recovery) — collects and returns the patient’s own blood during surgery. Reduces but does not eliminate transfusion need in major operations.
- Surgical haemostasis and minimising blood loss — technical strategies to reduce the extent of blood loss during procedure.
- HBOT — provides immediate plasma-dissolved oxygen to sustain tissue viability during the critical window when haemoglobin is at its lowest and EPO/iron have not yet taken effect.
HBOT is not a compromise within bloodless medicine. It is a scientifically validated tool — providing plasma-dissolved oxygen at levels that sustain tissue until the body’s own erythropoiesis restores haemoglobin. Using HBOT within a bloodless medicine protocol is fully consistent with the principles of bloodless care. It does not involve blood products of any kind.
Where HBOT Fits in the Timeline
| Timeline | Intervention | What It Achieves |
|---|---|---|
| Immediately | HBOT sessions — 2 to 3 per day in critical anaemia | Plasma oxygenation sustains tissue viability at rest |
| Days 1–3 | IV iron therapy initiated; EPO administered | Substrate and stimulus for erythropoiesis provided |
| Days 3–7 | Reticulocyte response begins | Early signs of haemoglobin recovery — HBOT continues as bridge |
| Days 7–14 | Haemoglobin begins measurable recovery | HBOT frequency reduced as haemoglobin approaches safety threshold |
| Days 14–30 | Haemoglobin approaches adequate levels | HBOT discontinued when haemoglobin sufficient to sustain tissue independently |
| Ongoing | Oral iron and nutritional support | Sustained haemoglobin recovery and prevention of recurrence |
The HBOT Protocol for Severe Anaemia
Standard Parameters
- Pressure: 2.0 to 2.4 ATA — sufficient to achieve resting tissue oxygen requirements via plasma
- Session duration: 90 minutes of pure oxygen breathing
- Frequency in critical phase: 2 to 3 sessions per day — every 6 to 8 hours — to maintain plasma oxygenation throughout the critical window
- Tapering: frequency reduced as haemoglobin recovers toward 7 to 8 g/dL
- Discontinuation: when haemoglobin is sufficient to sustain tissue oxygen delivery independently
Patient Monitoring During HBOT
- Haemoglobin and haematocrit checked before each session in critical anaemia
- Oxygen saturation monitored continuously during sessions
- Signs of organ hypoxia assessed — mental status, urine output, cardiac rhythm
- Blood glucose monitored — HBOT can occasionally cause mild hypoglycaemia
| UHMS Recognition | |
| Clinical Recognition | The Undersea and Hyperbaric Medical Society formally recognises acute anaemia with exceptional blood loss — where transfusion is not possible — as an HBOT indication. This recognition applies both to medical contraindication situations and to patients who decline transfusion for personal reasons. The clinical standard is identical regardless of the reason for transfusion unavailability. |
Severe Anaemia, Bloodless Medicine, and HBOT in India
India carries a substantial burden of severe anaemia — driven by nutritional deficiency (iron, B12, folate), haemoglobinopathies (sickle cell disease and thalassaemia are particularly prevalent), and blood loss from obstetric complications and trauma.
The Jehovah’s Witness community in India numbers in the hundreds of thousands. For this population — and for other patients with medical contraindications to transfusion — awareness of HBOT as a recognised bloodless medicine tool is critically low among both patients and treating physicians.
Post-partum haemorrhage is a leading cause of maternal mortality in India. For women who survive the acute blood loss event but present with critically low haemoglobin, HBOT provides a bridge while erythropoiesis recovers — a particularly important application in a country where obstetric haemorrhage outcomes remain a public health priority.
HBOT for severe anaemia is available at hospital-based hyperbaric units across major Indian metros. For facility information see our guides to HBOT in Delhi and HBOT in Bangalore. For the related plasma oxygenation mechanism, see our article on acute arterial insufficiency and HBOT.
 HBOT severe anaemia bloodless medicine — plasma oxygenation without transfusion bridge therapy
HBOT severe anaemia bloodless medicine — plasma oxygenation without transfusion bridge therapy
Frequently Asked Questions
Does HBOT involve blood or blood products?
No. HBOT involves no blood or blood products of any kind. The patient breathes 100% pure oxygen inside a pressurised chamber. The mechanism — plasma-dissolved oxygenation — occurs entirely within the patient’s own blood, using the liquid plasma component rather than red blood cells. This makes HBOT fully compatible with bloodless medicine principles and with personal or religious objections to blood transfusion.
How low does haemoglobin need to be before HBOT is indicated?
HBOT for anaemia is typically indicated when haemoglobin falls below 5 to 7 g/dL and transfusion is not possible — the threshold where tissue oxygen delivery is critically impaired despite maximum cardiovascular compensation. In practice, HBOT is initiated when clinical signs of tissue hypoxia are present — confusion, cardiac compromise, oliguria — regardless of the exact haemoglobin number.
How many sessions are needed?
The course length is entirely dependent on the rate of haemoglobin recovery. In acute post-haemorrhagic anaemia with normal bone marrow function and adequate iron/EPO support, haemoglobin typically begins recovering within 5 to 7 days and reaches safety thresholds within 2 to 4 weeks. HBOT sessions continue until haemoglobin is sufficient to sustain tissue without the plasma-dissolved oxygen bridge — typically at 7 to 8 g/dL. Session frequency is reduced progressively as haemoglobin rises.
How many sessions are needed?
The course length is entirely dependent on the rate of haemoglobin recovery. In acute post-haemorrhagic anaemia with normal bone marrow function and adequate iron/EPO support, haemoglobin typically begins recovering within 5 to 7 days and reaches safety thresholds within 2 to 4 weeks. HBOT sessions continue until haemoglobin is sufficient to sustain tissue without the plasma-dissolved oxygen bridge — typically at 7 to 8 g/dL. Session frequency is reduced progressively as haemoglobin rises.
Is HBOT safe for patients with severe anaemia?
Yes — with appropriate monitoring. Patients with severe anaemia may have compromised cardiovascular status, and sessions should be conducted with continuous monitoring of oxygen saturation, cardiac rhythm, and vital signs. The chamber environment and HBOT itself do not exacerbate anaemia. Hypoglycaemia risk should be monitored in patients who are nutritionally compromised. A qualified HBOT physician should assess suitability before initiating treatment.
Can HBOT be used for sickle cell anaemia crises?
HBOT has been explored in sickle cell disease as both an acute crisis intervention — reducing sickling by maintaining high tissue oxygen tension — and as a prophylactic measure. The evidence base is smaller than for acute blood loss anaemia, but physiological rationale is strong: high plasma oxygen tension reduces the sickling tendency of haemoglobin S. This application requires discussion with a haematologist and an HBOT physician jointly.
Does HBOT replace the need for iron and EPO therapy?
No. HBOT and iron/EPO therapy address different aspects of the problem. HBOT sustains tissue oxygen delivery in the immediate term — buying time while haemoglobin recovers. Iron and EPO therapy stimulate that recovery. Both are required. HBOT without iron/EPO support bridges the gap but does not close it. Iron and EPO without HBOT may not keep tissue viable during the lag period before haemoglobin responds. The combination is the complete bloodless medicine approach.
A Medically Sound Option That Respects Every Patient
The situation of not being able to receive a transfusion — for any reason — can feel like medicine has run out of options. It has not.
HBOT is not an improvised workaround. It is not experimental. It is a formally recognised UHMS indication, a component of bloodless medicine protocols at leading hospital centres globally, and a therapy whose mechanism — Henry’s Law applied clinically — is as settled as any science in medicine.
For Indian patients and families navigating this situation: the knowledge that this option exists is itself valuable. Asking your treating team about HBOT is not asking for something unusual. It is asking for the standard of care for this indication.
For the complete explanation of how HBOT delivers oxygen through plasma — the mechanism that makes bloodless oxygenation possible — visit How HBOT Works.
For related conditions where plasma oxygenation is critical, read our articles on arterial gas embolism and acute arterial insufficiency.
For insurance and cost guidance in India, see our HBOT insurance guide.
Your values and your medical care can align. The option exists. It is recognised. It is available.Explore the HBOTLAB Knowledge Centre →