Hyperbaric Oxygen Therapy Benefits and Risks for Diabetic Patients: The Complete Guide
Diabetes and HBOT are not at odds. They are complementary. The conditions that make diabetes dangerous — hypoxia, poor circulation, impaired healing — are precisely the conditions that hyperbaric oxygen therapy is designed to address.

hyperbaric oxygen therapy benefits and risks diabetes — HBOT diabetic patient safety guide India
Hyperbaric oxygen therapy benefits and risks for diabetic patients are not evenly understood — and that imbalance costs people their health.
The risks are talked about more than the benefits — even though, for diabetic patients specifically, the benefit profile is among the strongest of any patient group receiving HBOT. Diabetic tissue is hypoxic. Diabetic wounds do not heal. Diabetic nerves are starving. These are precisely the biological conditions that hyperbaric oxygen therapy addresses most directly.
The risks are real but manageable. Blood glucose requires monitoring. Insulin doses may need adjustment on treatment days. A handful of contraindications apply. But for the vast majority of diabetic patients, these are protocol requirements — not barriers to treatment.
This article is the complete guide for diabetic patients and their families evaluating HBOT. What the therapy does, what it reliably improves, what to watch for, and how to approach treatment safely.
For the foundational mechanism behind how HBOT delivers oxygen under pressure, visit How HBOT Works.
Why diabetics are prime HBOT candidates: Diabetes progressively damages small blood vessels, reducing oxygen delivery to peripheral tissue. This creates the chronic tissue hypoxia that HBOT specifically corrects — making diabetic patients among the most likely to benefit from hyperbaric oxygen therapy, and among the most important to treat.
Hyperbaric Oxygen Therapy Benefits for Diabetic Patients — Five Documented Areas
Benefit 1 — Diabetic Foot Wound Healing
Non-healing diabetic foot ulcers are the most extensively studied HBOT indication in diabetic populations — and the evidence is the strongest of all five benefit areas.
A comprehensive review by assessed HBOT for diabetic foot ulcers across multiple randomised controlled trials. Findings: significantly higher rates of wound healing, lower amputation rates, and improved limb salvage in HBOT groups compared to standard care alone.
The detailed evidence and treatment protocol for diabetic wound healing is covered in our full guide on HBOT for diabetic foot wounds.
Benefit 2 — Peripheral Neuropathy
Diabetic peripheral neuropathy — nerve damage caused by hypoxic microvasculature — is the leading cause of diabetic amputation globally. HBOT restores oxygen to hypoxic nerve tissue and stimulates angiogenesis in the damaged nerve bed.
Clinical improvement in nerve conduction velocity, vibration perception threshold, and pain scores has been documented in patients with early to intermediate neuropathy after HBOT courses of 20 to 40 sessions.
Our detailed guide on hyperbaric therapy for neuropathy covers the neuropathy-specific mechanism and evidence.
Benefit 3 — Microvascular Circulation Improvement
Beyond wounds and nerves, HBOT stimulates new blood vessel formation throughout the body — not only at the wound site. documented that HBOT mobilises vasculogenic stem cells and stimulates VEGF-driven neovascularisation — creating a systemic improvement in microvascular supply that benefits all diabetic tissue over a treatment course.
For diabetic patients with peripheral vascular disease, this angiogenesis benefit is clinically meaningful beyond wound healing — improving peripheral circulation in the feet and legs broadly, not only at specific wound sites.
Benefit 4 — Infection Resistance
Diabetic tissue is highly susceptible to infection — poor circulation impairs immune cell delivery and function, and hypoxic tissue provides an hospitable environment for bacteria. HBOT creates a high-oxygen tissue environment hostile to anaerobic bacteria and restores leukocyte killing capacity to levels that effective infection control requires.
For diabetic patients with infected ulcers, osteomyelitis, or post-surgical wound infections, HBOT’s anti-infective benefit operates alongside antibiotics — restoring the tissue oxygen that makes antibiotic therapy effective in hypoxic diabetic tissue.
Benefit 5 — Reduced Amputation Risk
All four benefits above converge on a single outcome: amputation prevention. Wounds heal instead of progressing. Nerves preserve protective sensation. Circulation improves in at-risk tissue. Infections resolve instead of advancing to osteomyelitis.
documented reduced major amputation rates in diabetic foot ulcer patients who received HBOT. This is the single most clinically important outcome measure for diabetic HBOT — and the one that justifies its use as a proactive rather than last-resort intervention.
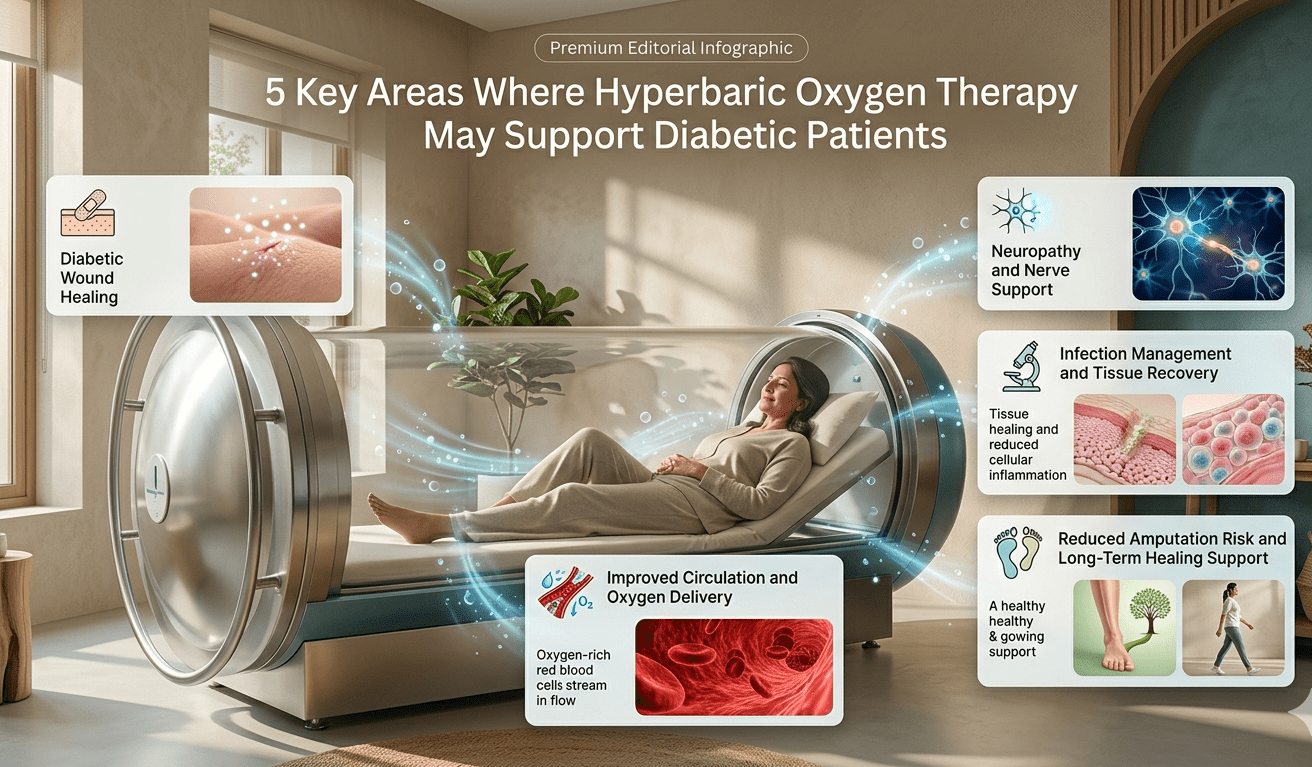
hyperbaric oxygen therapy benefits diabetes — five areas wounds neuropathy circulation infection amputation
Hyperbaric Oxygen Therapy Risks for Diabetic Patients — What to Know
The risk profile of HBOT for diabetic patients is well-understood and manageable. The specific risks that apply to diabetic populations are distinct from the general HBOT risk profile — and all are addressed through standard protocol.
| Risk | Why It Applies to Diabetic Patients | How It Is Managed |
| Hypoglycaemia during sessions | HBOT increases cellular glucose metabolism. Insulin-dependent diabetics may experience blood glucose drop during or after sessions. | Blood glucose checked before every session. Insulin dose adjustment on treatment days. Glucose available in chamber. |
| Delayed wound recognition | Neuropathy reduces sensation — minor pressure injuries from chamber positioning may go unnoticed. | Thorough skin inspection before and after every session. Padding for bony prominences. Staff awareness of neuropathy status. |
| Cataract progression | Diabetics already have higher cataract risk. Long HBOT courses (40+ sessions) may marginally accelerate this in some patients. | Ophthalmology baseline assessment for long courses. Benefit-risk assessment with treating physician. |
| Barotrauma — ear and sinus | Higher risk in patients with diabetic autonomic neuropathy affecting Eustachian tube function. | Slow pressurisation. Equalisation guidance. Decongestant use if required. |
| Oxygen toxicity | No specific additional risk for diabetic patients vs general population at standard pressures. | Standard air breaks in protocol. Seizure risk <1 in 10,000 sessions at 2.0–2.4 ATA. |
| The Key Point on Risks | None of the risks above are reasons to withhold HBOT from diabetic patients. They are protocol requirements — adjustments that are standard practice at any competent hyperbaric facility. The benefit-risk ratio for diabetic patients with foot ulcers, neuropathy, or poor peripheral circulation strongly favours treatment with appropriate monitoring. |
Contraindications — Diabetic Patients Who Should Not Receive HBOT
A small number of contraindications apply to all HBOT patients, some of which are relevant to diabetic populations.
Absolute Contraindications
- Untreated pneumothorax — must be drained before HBOT. Diabetic patients with respiratory complications should be assessed.
- Certain chemotherapy agents — bleomycin and doxorubicin have specific HBOT interactions. Relevant for diabetic cancer patients.
Relative Contraindications — Require Physician Assessment
- Uncontrolled blood glucose above 250 mg/dL — HBOT should not begin until glucose is stabilised. Hyperglycaemia increases oxygen toxicity risk and reduces HBOT efficacy.
- Active proliferative diabetic retinopathy — theoretical concern about oxygen effects on retinal neovascularisation. Ophthalmology assessment recommended before HBOT in patients with active proliferative disease.
- Severe claustrophobia — manageable in many cases with anxiolytic medication. Multiplace chambers offer a less enclosed environment.
Before Starting HBOT — What Diabetic Patients Need to Do
Step 1 — Get Blood Glucose Under Control
HBOT works best in well-controlled diabetic tissue. Chronic hyperglycaemia continues to damage the microvessels that HBOT is trying to restore. Optimising HbA1c before and during HBOT treatment maximises the therapy’s effectiveness. This is not a prerequisite that delays treatment — it is a parallel priority that improves outcomes.
Step 2 — Coordinate Your Care Team
Your diabetologist, wound care specialist, and hyperbaric physician need to communicate. Insulin dosing on treatment days, wound dressing protocols, and monitoring frequency all require coordination. The best outcomes from HBOT in diabetic patients come from integrated care — not HBOT as an isolated intervention.
Step 3 — Know What to Monitor
- Blood glucose before every session — standard protocol at any qualified facility
- Skin condition at all pressure points — feet, heels, and bony prominences inspected before and after each session
- Wound progress — measured and documented at regular intervals throughout the course
- Visual symptoms — any changes in vision during a long HBOT course warrant ophthalmology review
HBOT for Diabetic Patients in India — Access and Cost
India has approximately 77 million diabetic patients — the world’s second-largest diabetic population. Of these, approximately 15% will develop a foot ulcer during their lifetime, and 25% of foot ulcers will progress to amputation without adequate treatment. HBOT, used appropriately in the diabetic wound and neuropathy context, addresses the upstream biology that drives this outcome.
HBOT for diabetic complications is available at hospital-based units and dedicated wellness centres across Delhi NCR, Mumbai, Bangalore, Hyderabad, and Chennai. Coverage under insurance schemes remains limited but is growing for specific FDA-recognised indications including diabetic foot ulcers.
For facility locations see our guides to HBOT in Delhi and HBOT in Bangalore. For cost information, see our HBOT cost guide. For insurance, see our HBOT insurance India guide.
Frequently Asked Questions
Is HBOT safe for Type 1 diabetics on insulin?
Yes — with blood glucose monitoring before every session and insulin dose adjustment on treatment days. Insulin-dependent patients are treated routinely at hyperbaric centres globally. The protocol is established and well-understood. Type 1 diabetics on insulin may need a reduced dose on treatment days as HBOT increases cellular glucose uptake. Your HBOT physician and diabetologist should coordinate on this before the first session.
Is HBOT safe for Type 2 diabetics on oral medication?
Yes. Oral hypoglycaemic agents do not require adjustment in most cases. Blood glucose should still be monitored before each session. The hypoglycaemia risk is lower for patients on oral agents than for those on insulin, but monitoring remains standard protocol regardless of medication type.
Can HBOT help if I have had a diabetic foot amputation?
Yes — in two ways. For the post-amputation wound and stump, HBOT supports healing by oxygenating the wound bed and reducing infection risk. For the remaining limb, HBOT addresses the same neuropathy and microvascular disease that caused the first amputation — improving circulation, preserving sensation, and reducing the risk of a second amputation.
How long does a course of HBOT take for a diabetic patient?
Wound healing: typically 30 to 40 sessions, five days per week — approximately 6 to 8 weeks. Neuropathy management: 20 to 40 sessions depending on severity and response. The treating team should assess wound healing progress at session 20 and adjust the course accordingly. Patients who respond well may complete the course at session 30. Those with extensive disease may require 40 or more.
Will HBOT interfere with my diabetes medications?
For most diabetes medications — metformin, DPP-4 inhibitors, SGLT-2 inhibitors, GLP-1 agonists — no specific interactions with HBOT are documented. Insulin is the primary medication requiring dose adjustment. Your HBOT physician should receive a complete medication list before treatment begins and coordinate with your diabetologist on any adjustments needed.
Diabetes and HBOT — The Right Question Is Not Whether, But When
The question most diabetic patients ask when they encounter HBOT is: is it safe for me? The honest answer is yes — with the protocols and monitoring that any qualified facility applies as standard.
The more important question is: when should I start? For diabetic patients with established foot ulcers, the answer is now. For patients with early neuropathy, the answer is before the wound forms. For patients with poor peripheral circulation and no active wound, the answer is before the complication becomes irreversible.
Hyperbaric oxygen therapy benefits and risks for diabetic patients are well-documented across decades of research. The benefits are substantial and condition-specific. The risks are manageable with protocol. The outcomes — wound healing, nerve preservation, limb salvage — are among the most meaningful in diabetic care.
For the full conditions evidence base, see our HBOT conditions reference. For the complete diabetic wound healing evidence, read our guide on HBOT for diabetic foot wounds.
The biology of diabetic tissue responds to oxygen. HBOT delivers it. The decision to start is the first step.