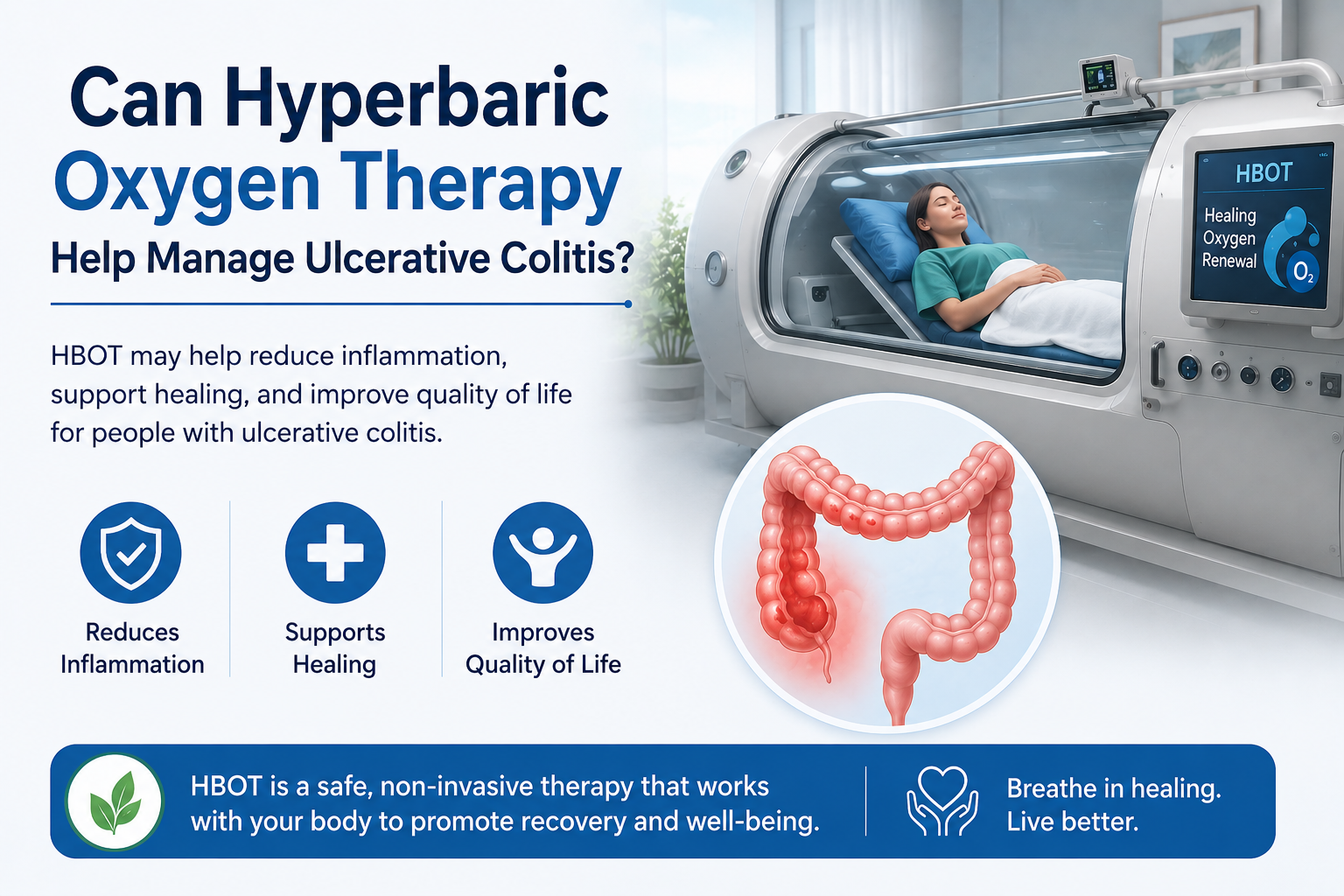
Can Hyperbaric Oxygen Therapy Help Manage Ulcerative Colitis?
Living with Ulcerative Colitis often feels like navigating a cycle of flare-ups, fatigue, and uncertainty. For many patients, standard treatments such as anti-inflammatory drugs, immunosuppressants, and biologics offer relief—but not always complete control. This gap has led both patients and clinicians to explore adjunct therapies that may support healing beyond conventional care.
One such emerging option is Hyperbaric Oxygen Therapy. At HBOTLAB, interest in this therapy continues to grow as individuals seek non-invasive ways to complement their existing treatment plans. The question remains: can it genuinely help manage ulcerative colitis?
What Happens in Ulcerative Colitis?
Ulcerative colitis (UC) is a chronic inflammatory condition affecting the colon and rectum. It causes the inner lining of the large intestine to become inflamed, leading to ulcers, bleeding, and discomfort. Symptoms can vary but often include:
- Persistent diarrhea, sometimes with blood
- Abdominal pain and cramping
- Urgency to pass stool
- Fatigue and weight loss
- Reduced appetite
The root cause involves an abnormal immune response where the body mistakenly attacks its own intestinal tissue. Over time, this leads to cycles of damage and repair, often without complete healing.
The Science Behind Hyperbaric Oxygen Therapy
Hyperbaric Oxygen Therapy involves breathing pure oxygen inside a pressurized chamber. Under these conditions, oxygen dissolves more effectively into the bloodstream, reaching tissues that may otherwise be oxygen-deprived.
This increased oxygen availability supports several physiological processes:
- Enhanced tissue repair and regeneration
- Reduced inflammation
- Improved immune response
- Promotion of new blood vessel formation (angiogenesis)
- Faster wound healing
For conditions involving chronic inflammation and poor tissue oxygenation—like Ulcerative Colitis—these mechanisms offer promising therapeutic potential.
Why Oxygen Matters in Ulcerative Colitis
Inflamed intestinal tissues in UC patients often suffer from reduced oxygen supply. This creates a challenging environment for healing. Low oxygen levels can:
- Delay tissue repair
- Increase oxidative stress
- Worsen inflammation
- Disrupt the gut lining barrier
By delivering high concentrations of oxygen directly to affected tissues, Hyperbaric Oxygen Therapy for Ulcerative Colitis aims to reverse these conditions and support recovery at a cellular level.
Potential Benefits of Hyperbaric Oxygen Therapy for Ulcerative Colitis
1. Reduction in Inflammation
Chronic inflammation is the driving force behind UC symptoms. HBOT has been shown to reduce pro-inflammatory cytokines, helping to calm the immune response.
2. Accelerated Healing of Ulcers
Ulcers in the colon can take time to heal due to ongoing inflammation and limited oxygen supply. HBOT enhances oxygen delivery, promoting faster regeneration of damaged tissues.
3. Improved Gut Barrier Function
The intestinal lining acts as a protective barrier. When compromised, it allows harmful substances to pass through. Oxygen therapy supports the repair of this lining, strengthening its function.
4. Decreased Frequency of Flare-Ups
While not a cure, consistent HBOT sessions may help stabilize symptoms and reduce the recurrence of flare-ups when used alongside medical treatment.
5. Enhanced Quality of Life
Less pain, improved digestion, and increased energy levels contribute to a better overall lifestyle for patients managing UC.
Clinical Insights and Research Direction
Research into Hyperbaric Oxygen Therapy for Ulcerative Colitis is still evolving, but early findings are encouraging. Clinical observations suggest that patients undergoing HBOT may experience:
- Reduced disease severity scores
- Improved mucosal healing seen in colonoscopy
- Lower dependency on steroids in some cases
These outcomes highlight HBOT’s role as a supportive therapy rather than a replacement for conventional treatments.
Who May Benefit from HBOT?
Not every UC patient requires advanced therapies, but HBOT may be considered in specific cases:
- Individuals with moderate to severe UC
- Patients not responding well to medication
- Those experiencing frequent relapses
- Individuals seeking non-invasive complementary care
At HBOTLAB, therapy plans are tailored after evaluating individual health conditions, ensuring safety and effectiveness.
What to Expect During a Session
A typical HBOT session is simple and non-invasive:
- The patient enters a specialized chamber
- Pressure gradually increases
- Pure oxygen is administered
- Sessions usually last 60–90 minutes
- Multiple sessions may be recommended over weeks
Patients often report a relaxing experience, similar to resting in a quiet, controlled environment.
Safety and Considerations
Hyperbaric Oxygen Therapy is generally safe when administered under professional supervision. However, certain precautions are essential:
- Not suitable for untreated pneumothorax
- Requires monitoring in patients with respiratory conditions
- Mild side effects may include ear pressure or temporary fatigue
At HBOTLAB, strict safety protocols are followed to ensure every session is conducted under expert care.
Integrating HBOT with Conventional Treatment
It’s important to view Hyperbaric Oxygen Therapy for Ulcerative Colitis as a complementary approach. It works best when integrated with:
- Prescribed medications
- Nutritional support
- Stress management strategies
- Regular medical supervision
This combined approach addresses both symptoms and underlying triggers, offering a more balanced path to managing UC.
Diet, Lifestyle, and Oxygen Therapy
Therapy outcomes can improve significantly when paired with supportive lifestyle changes:
- Eating anti-inflammatory foods
- Staying hydrated
- Managing stress through mindfulness or light exercise
- Avoiding known dietary triggers
HBOT enhances the body’s natural healing ability, and these habits create an environment where healing can thrive.
The Role of HBOTLAB
At HBOTLAB, the focus is on delivering advanced oxygen therapy solutions backed by expertise and personalized care. Each treatment plan is designed to align with the patient’s medical history and current condition.
Patients receive:
- Individualized therapy protocols
- Professional supervision
- Comfortable and safe treatment environments
- Ongoing support throughout the therapy cycle
The goal is not just symptom management, but improving long-term wellness.
Limitations to Keep in Mind
While promising, HBOT is not a standalone cure for ulcerative colitis. Patients should remain realistic about outcomes:
- Results may vary from person to person
- Long-term effectiveness requires further research
- Continued medical treatment is necessary
Clear communication with healthcare providers ensures the best possible results.
Looking Ahead
Interest in Hyperbaric Oxygen Therapy continues to expand across multiple medical fields. For chronic inflammatory conditions like Ulcerative Colitis, its role is gradually becoming more defined.
Ongoing research and patient experiences will continue to shape how this therapy is integrated into treatment plans. As awareness grows, more individuals are exploring it as part of a broader strategy for managing chronic health conditions.
Final Thoughts
Managing ulcerative colitis requires persistence, patience, and a willingness to explore supportive therapies. Hyperbaric Oxygen Therapy for Ulcerative Colitis presents a scientifically grounded option that focuses on healing from within—by improving oxygen delivery, reducing inflammation, and supporting tissue repair.
For those seeking additional support beyond traditional treatments, HBOTLAB offers a structured and professional approach to oxygen therapy. While it may not replace existing medical care, it has the potential to enhance outcomes and improve day-to-day living.